
Makes mealtimes fun

For everyday strolls with a one hand fold



Add Muslin Swaddles worth £45 for FREE!

Suitable from newborn to toddler, Pop is the ultimate everyday pushchair offering a smooth and comfortable ride for baby and added peace-of-mind for parents.
The place for parents to be
Min read
Min read
Min read
Min read
Min read

Coast is our cool and durable carrycot/pushchair travel system which features stylish detailing and premium marl fabrics. Coast is fully accessorised with a co-ordinating deeply padded footmuff and super practical pram bag.

Tide is our new multi-terrain pushchair with an overnight sleeping approved carrycot, reversible multi-recline pushchair seat and effortless freestanding fold.

Introducing the all new Wave, our future-proof travel system that’s designed especially for growing families.

Suburban, stylish, sustainable – Reef is our multi-terrain travel system offering the ultimate in baby comfort no matter where your adventures take you.

Dune, our contemporary and compact urban travel system proves there’s no need to compromise when it comes to style and functionality.

Add an award-winning Dream i-Size Infant Carrier & Base with your Coast pushchair, designed for everyday strolls

Our lightest, most compact multi-terrain pushchair, Tide is made for exploring. Includes Accessory pack with a changing rucksack, footmuff, phone holder and cup holder.

Our lightest, most compact multi-terrain pushchair, Tide is made for exploring. With 4-wheel suspens...

Our lightest, most compact multi-terrain pushchair, Tide is made for exploring. With 4-wheel suspens...

Everything you need with your Wave pram including Dream i-Size infant carrier & base, changing bag, footmuff, phone holder and snack tray

Turn your Wave pram into a Travel System with an award-winning Dream i-Size infant carrier

Everything you need with your Reef pram including a First Bed Folding Carrycot, Dream i-Size infant carrier, changing bag, footmuff, phone holder and snack tray

Reef, our multi-terrain travel system offering the ultimate in baby comfort no matter where your adventures take you with its freestanding fold, first bed folding carrycot and off road wheels with a travel pack

Everything you need with your Dune pram including a First Bed Folding Carrycot, Dream i-Size infant carrier, changing bag, footmuff, phone holder and snack tray

Combine your Dune pram with a Newborn Pod and an award-winning Dream i-Size infant carrier and Travel pack.

Everything you need with your Dune pram including a Compact Folding Carrycot, Dream i-Size infant carrier, changing bag, footmuff, phone holder and snack tray

Combine your Dune pram with a Compact Folding Carrycot and an award-winning Dream i-Size infant carrier

For everyday strolls with a one hand fold

Suitable from newborn to toddler, Pop is the ultimate everyday pushchair offering a smooth and comfortable ride for baby and added peace-of-mind for parents.

Upgrade your daily strolls with Zest, our everyday pushchair offering style and comfort for both parents and babies.
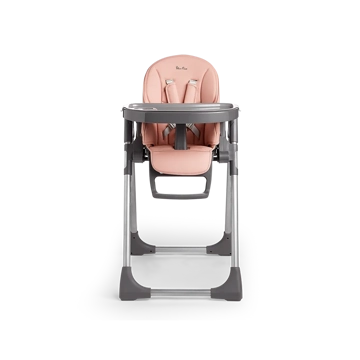
Makes mealtimes fun

Eat&Play is the 4-in-1 highchair and play table that does it all. Transforming effortlessly from...

For snacking, weaning and playtime
Start you little one's weaning journey

Awarded the safest infant carrier for your newborn by ADAC, when used with the Dream i-Size base

The only 360° rotating car seat you need, suitable from birth to approx. 12 years

The multi-stage car seat, growing with your child from 15 months to approx. 12 years of age

Our high-back booster seat from 4 to 12 years old, approved to the latest R129/03 safety standard

Simple and beautiful, the Bromley nursery furniture collection offers the perfect canvas for creatin...

Create the best nursery for your little one to nap, play and grow with the Bromley Oak 3-piece nurse...

Special edition auto-folding super stroller.

Special edition 360° rotating, all stage car seat.

Special edition one-pop travel cot, co-sleeper and playpen.
Like so many women, I always dreamt of having a peaceful water birth, welcoming my baby earthside in this bubble of serenity.
But after a traumatic first birth experience with my son and a series of events that led to us moving homes at 38 weeks pregnant, I really wasn’t sure I was in the frame of mind to embrace a ‘natural’ birth with my daughter Lilah.
However, my top priority was to feel empowered in my choices this time around. So, I read far and wide, listened to every podcast under the sun and enveloped myself in a cocoon of positive birth stories.
The night of Lilah’s due date, I remember going to bed feeling quite disheartened that she had not given even an inkling of her impending arrival. My son was born exactly on his due date so it never crossed my mind that my daughter could possibly come later.
She did. But not by much.

10/01/2020, 6:30 AM
The morning after my due date I woke up early with contractions. I immediately felt that rush of excitement and nerves and wonderful certainty that I would soon meet my daughter. Still, I expected things to progress very slowly. My first labour was 14 hours and I felt confident I knew exactly what lay ahead. And that this would undoubtedly be quite slow. I called my sister to make the 1.5-hour drive to us in West London to watch my son, so my partner Mathew and I were ready to head to the hospital. The morning was very ordinary - I wore one of my favourite dresses, pottered around the house and tended to my son. With contractions coming in regularly but very manageable, I breathed through them, feeling them ebb and flow like waves, exactly the way I had prepared for.
10:30 AM
Mathew had arranged for his car to be picked up on exactly this day so I remember the car salesman being at the front door joking: “You’re not giving birth yet, are you?” as I breathed through another contraction with what must have been a pretty pained look on my face. “No, no we still have hours to go”, I laughed and continued tending to my son as contractions got stronger. It was all still very calm and I felt in control and at peace.

11:20 AM
My waters broke. Suddenly, things got more intense. I rushed to the bathroom to change, thought about taking a warm shower to help ease the pain but contractions were increasing in intensity and frequency so quickly now I didn’t even manage to finish that thought. I could hear my sister had arrived and shouted for Mathew to get a cab NOW. An epidural crossed my mind, thinking I couldn’t possibly endure another 8-10 hours of this pain, no matter how much I had prepared to breathe through it. I knelt on all fours in the bathroom and felt disorientated by this sudden intense pain, thinking back to everything I had read and telling myself surely, I still had plenty of time to go before I should feel this way. Another intense contraction gripped me so hard I threw up.

11:30 AM
At this point I knew. I shouted for Mathew to call an ambulance. He later told me he thought I was being over dramatic as he felt we still had hours to go. But he opened the lock of our tiny bathroom, kneeled in front of me as I gripped his shoulders and dialled 999. A sudden state of panic started to set in as I realised that we would be delivering this baby alone. I was almost in a trance. A panicked trance. I never thought I would be very vocal during birth as I’m generally more the quiet type, but Mathew might beg to differ that labour definitely confirmed otherwise. I screamed with each contraction. Maybe out of panic, maybe out of instinct, maybe both. Looking back it was almost that primal image of birth most people probably have when picturing it.
I hardly remember what the 999 operator was saying but there was a blur of turning around on my back to deliver baby when Mathew noticed the head coming out and I remember feeling quite annoyed, wanting to stay on all fours where I felt comfortable. The thing I do remember distinctly is there was no need to actually push. At this point, I felt contractions completely take over my body and everything happened so naturally.
11:40 AM
Lilah was born, caught in her father’s arms. He laid her straight on my chest. The 999 operator was still instructing him as we rubbed her dry with towels, waiting for her to take her first breath. It took a few moments until we heard that first precious cry. Mathew was just about to go and find a shoelace to tie the cord when paramedics arrived. And I laid on our bathroom floor, still wearing the same dress I had worn all morning, covered in blood and vernix in complete disbelief that I had just delivered our baby at home – accidentally. And completely unassisted.
From then on, things are a bit of a blur. We were waiting for the placenta to be delivered but it never did, so the decision was made to go to the hospital. Thankfully I was able to deliver the placenta there and just needed some stitches – ouch! A few hours later, we were already back at home, curled up on the sofa with my sister recounting the crazy experience with some Domino’s pizza, going “I can’t believe this happened!”
Writing this, almost two years later, I still can’t quite believe it. Out of all the lessons that giving birth has taught me, including that it never goes to plan (!), the biggest would probably be to trust my body. Although it definitely wasn’t the calm birth experience I had prepared for, my unassisted (accidental) home birth was the most empowering, redemptive experience that really changed the way I view birth and my own capabilities.

Veronika Brachmaier is a young mama of two, health visitor and founder of a children’s concept store. She shares her love for sustainable and ethical style with snippets of daily life regularly connecting with mamas over the highs and lows of motherhood.